Fibroids are common, often misunderstood, and too often dismissed. This guide breaks down what they are, how many women are affected, who is most at risk, the symptoms that can disrupt daily life, and the options for getting real help.
Quick note: If you’ve been told your pain is “normal,” you’re not alone. Heavy bleeding, anemia, pelvic pressure, and pain can be signs of fibroids and deserve medical attention.
What are uterine fibroids?
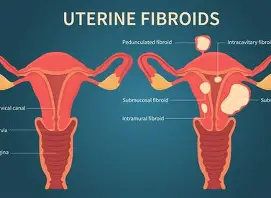
Uterine fibroids (also called leiomyomas) are non-cancerous growths made of muscle and connective tissue that develop in or on the uterus. They can be tiny like a seed or large enough to change the shape of the uterus. Some women have one; others have multiple.
Common symptoms (and why they can feel unbearable)
Many women have fibroids with no symptoms. But when symptoms happen, they can be life-altering.
- Heavy or prolonged periods (sometimes with clots)
- Anemia (low iron) from blood loss → fatigue, weakness, dizziness
- Pelvic pain/pressure or a heavy feeling in the lower belly
- Frequent urination (pressure on bladder)
- Constipation or rectal pressure
- Pain during sex
- Difficulty getting pregnant or pregnancy complications (in some cases)
- Bleeding so heavy you soak a pad/tampon every hour for 2+ hours
- Fainting, chest pain, severe shortness of breath, or severe weakness
- Sudden severe pelvic pain, fever, or suspected pregnancy complications
Who is more at risk?
Researchers don’t know one single cause, but fibroid growth is strongly influenced by hormones and genetics. Certain groups are more likely to develop fibroids, develop them earlier, and/or have more severe symptoms.
Higher-risk patterns
- Age: Risk increases through the reproductive years and often improves after menopause.
- Race: Black women are more likely to develop fibroids, often at younger ages, with more severe symptoms.
- Family history: Having a close relative with fibroids increases risk.
- Higher body weight/obesity is associated with increased risk.
- High blood pressure has been linked with higher risk in multiple resources.
- No history of pregnancy is listed as a risk factor in some guidance.
- Vitamin D deficiency is listed among risk factors in NICHD materials.
Diagnosis: what to expect at the doctor
Diagnosis often starts with a pelvic exam and a conversation about symptoms. Imaging is commonly used to confirm:
- Ultrasound (most common first test)
- MRI (more detail; helpful for planning treatment)
- Lab tests to check anemia/iron levels if heavy bleeding is present
Treatment options (you have choices)
The “best” option depends on your symptoms, fibroid size/location, age, medical history, and whether you want future pregnancy. Many women are offered hysterectomy early, but there are other paths worth discussing too.
Watchful waiting
If symptoms are mild, you may monitor fibroids over time with periodic exams/imaging.
Medication-focused options
- Hormonal birth control may help bleeding and cramps for some women.
- Other prescription options may be used to manage bleeding or temporarily shrink fibroids (your clinician can explain what fits your case).
- Iron supplements may be needed if anemia is present (with medical guidance).
Procedures & surgery
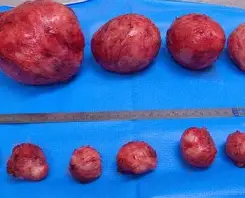
- Myomectomy: removes fibroids while keeping the uterus (often preferred when fertility is desired).
- Uterine artery embolization (UAE): reduces blood flow to fibroids to shrink them (not ideal for every fertility goal).
- Minimally invasive options may be available depending on fibroid type/location.
- Hysterectomy: removes the uterus; a definitive option, and a common one in fibroid care.
- Where are my fibroids located (inside the wall, on the outside, inside the cavity)?
- How might they impact bleeding, pain, and fertility?
- What are my uterus-sparing options?
- What recovery time should I expect for each option?
The quality-of-life impact (why this deserves attention)
Fibroids can affect work, relationships, mental health, confidence, sex life, and finances—especially when symptoms cause missed work, chronic pain, or repeated ER/doctor visits. Many women report years of being dismissed or told symptoms are normal.
Living with fibroids: practical support
- Track your symptoms (bleeding days, clot size, pain level, fatigue, bathroom trips).
- Ask for anemia testing if you have heavy bleeding or exhaustion.
- Bring receipts to appointments (symptom tracker, questions, goals, medication list).
- Get a second opinion if you feel dismissed or pressured into one option only.
FAQ
Are fibroids cancer?
Fibroids are usually benign (non-cancerous). If you have concerns about rapid growth or unusual symptoms, ask your clinician what signs require additional evaluation.
Can fibroids cause infertility?
Sometimes. It depends on size and location. Fibroids that distort the uterine cavity may affect implantation or pregnancy. Many women with fibroids still get pregnant, but it’s worth an individualized plan.
Do fibroids go away after menopause?
Fibroids often shrink after menopause due to reduced hormone levels, but this is not guaranteed for everyone, and symptoms should still be evaluated.
What should I say to my doctor if I’m not being heard?
Try: “My bleeding/pain is affecting my quality of life. I want a treatment plan and I want to discuss uterus-sparing options, too.” It can also help to bring a symptom log and ask for anemia testing.
You’re not “being dramatic.” You’re being honest.
Too many women carry this in silence. If you’re suffering, you deserve answers, options, and a provider who takes your pain seriously. Share this page with someone who needs it—and if you’re comfortable, talk about fibroids openly. Awareness helps women get diagnosed sooner.
Medical disclaimer: This article is for informational purposes only and does not replace medical advice. If you’re experiencing severe symptoms, seek medical care.
Wrap‑up: why “Generative Pre‑Trained Transformer” matters
Put simply: GPTs are strong writers and explainers because they’re trained on language patterns and powered by attention that keeps context in view. That combo lets them respond quickly, flexibly, and in many styles—while still needing human judgment for facts and high‑stakes decisions.


